
Partners
Offer your clients a complete range of HR management and compliance services by partnering with MyHRConcierge. We partner with banks, payroll providers, associations, insurance brokers, accountants, franchisors, and more.
Offer Your Clients High-Quality, Affordable HR Services
MyHRConcierge partner services provide your clients with the expertise to face any and all HR questions. The world of HR is filled with complex state and federal rules and compliance regulations.
MyHRConcierge partners with businesses across the United States to offer their clients a complete line of HR products and services that include:
- HR outsourcing services
- Benefits administration
- COBRA administration
- Employee screening solutions
- Employee handbooks
- …and more
What is Our Client Size and Location?
Our clients range from 5 employees to over 1,200 employees across the United States in industries such as:
- Grocery
- Manufacturing
- Hospitality
- Healthcare
- and more
“We sold over $3.5 million in MyHRConcierge services annually and didn’t have to worry about loss of clients due to the quality service.”
Buildable Partner Opportunities
Our flexible service offering provides you the ability to build a program that works best for you and your clients. It also provides opportunities for you to upsell to new products and services to increase your profits.
Learn more about the structure of our partnerships.
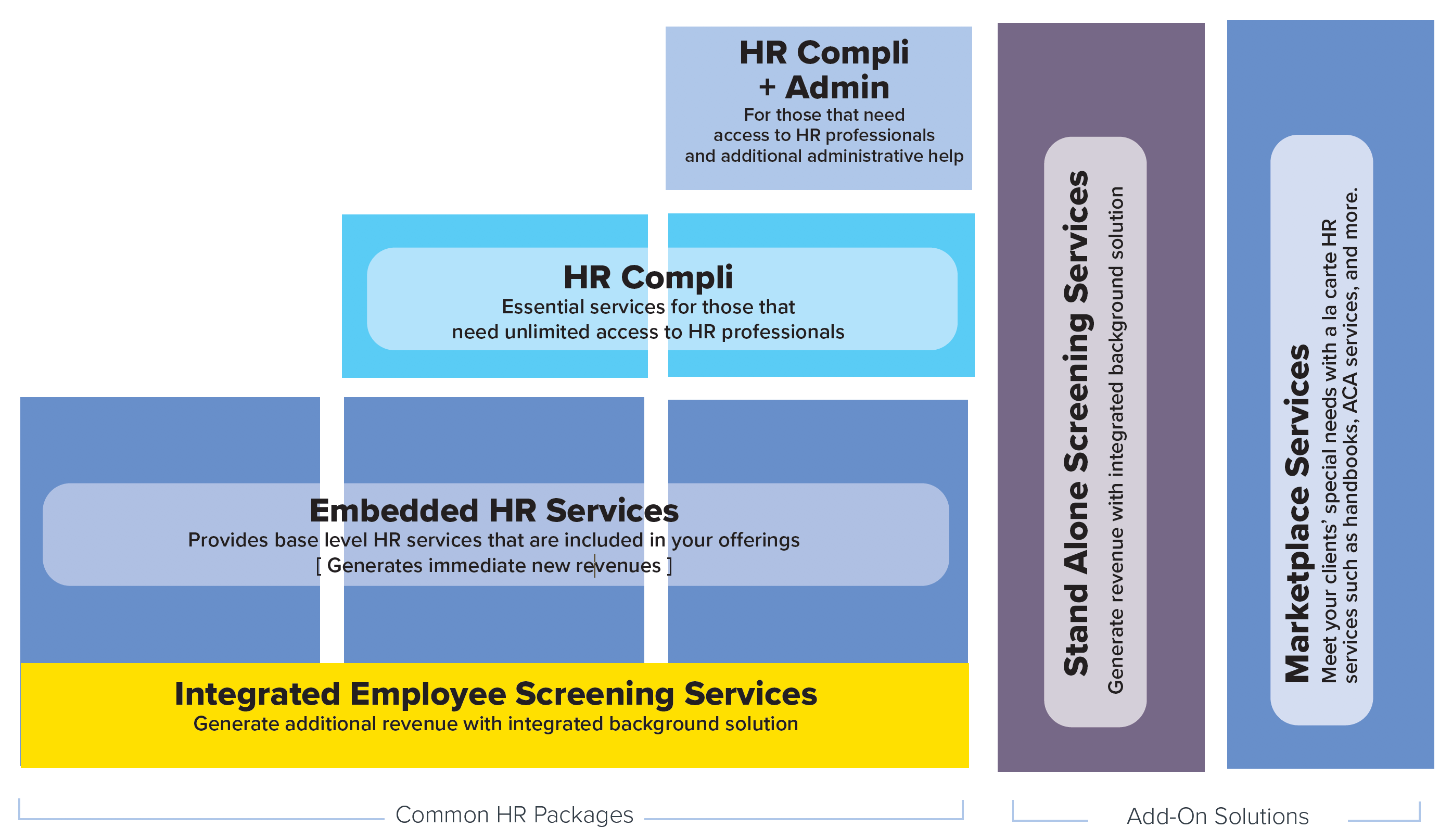
Embedded Services
Embedded services are low cost services that can be included in
existing offerings as an additional value to your clients.
HR Compliance Packages
Offers three levels of service to the end user. You’ll speak with a live
person that will support your HR related issues, administrative outsourcing and employee screening.
Marketing Support
As a partner we’ll work with your marketing team to develop a successful launch plan including ongoing support such as webinars, email blasts, shareable content, etc.
MyHRConcierge Increases Partner Opportunities
When you partner with us, we provide a wide variety of human resource and employee screening solutions to:
- Build additional revenue streams
- Differentiate you from the competition
- Increase client retention through additional services
Increase Your Revenue
We want to help you increase your profit by providing HR services that are flexible, competitive, and meet the needs of clients. These services can complement your existing product offering to help you increase your bottom line.
In addition to the profits from our HR services, you also create additional profit from an increase in client retention and new sales due to having a more diverse offering.
Contact MyHRConcierge
If you’d like to learn more about partnering with MyHRConcierge to offer your clients superior products and services and increase your revenue, contact us for a free consultation.
